How It Works
BTL Emsella is a breakthrough treatment that’s transforming pelvic health—offering a simple, non-invasive way to strengthen pelvic floor muscles and reduce issues like incontinence and sexual dysfunction. All you have to do is sit back and let the technology do the work.
How Does BTL Emsella work?
BTL Emsella is an innovative development in the field of pelvic health, changing women’s and men’s lives across the world. Using High-Intensity Focused Electromagnetic, (HIFEM) technology, BTL Emsella is one of the easiest, most relaxing, and non-invasive treatments available to help reduce urinary leakage and dribbles, and free women and men from incontinence and erectile dysfunction.
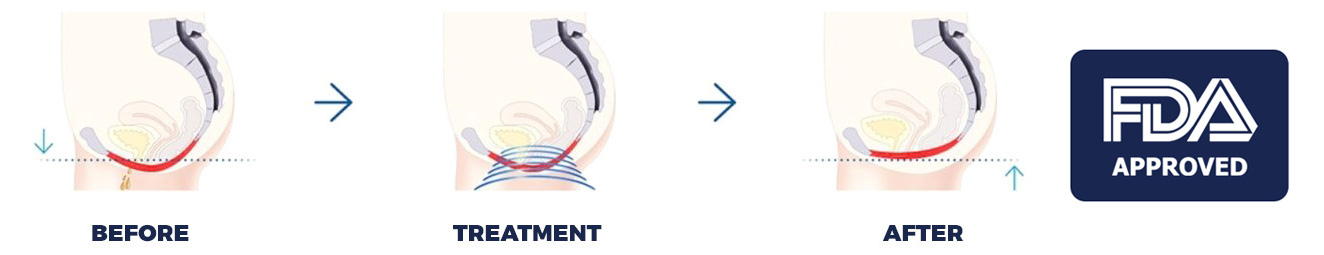
By the time you come in for a BTL Emsella treatment, you will likely have weak or atrophied muscle support around your pelvic floor. This is what causes many women and men to suffer embarrassing urinary incontinence or decreased sexual satisfaction. Strengthening these muscles, and helping them to become tighter will go a long way in improving the patients’ quality of life.
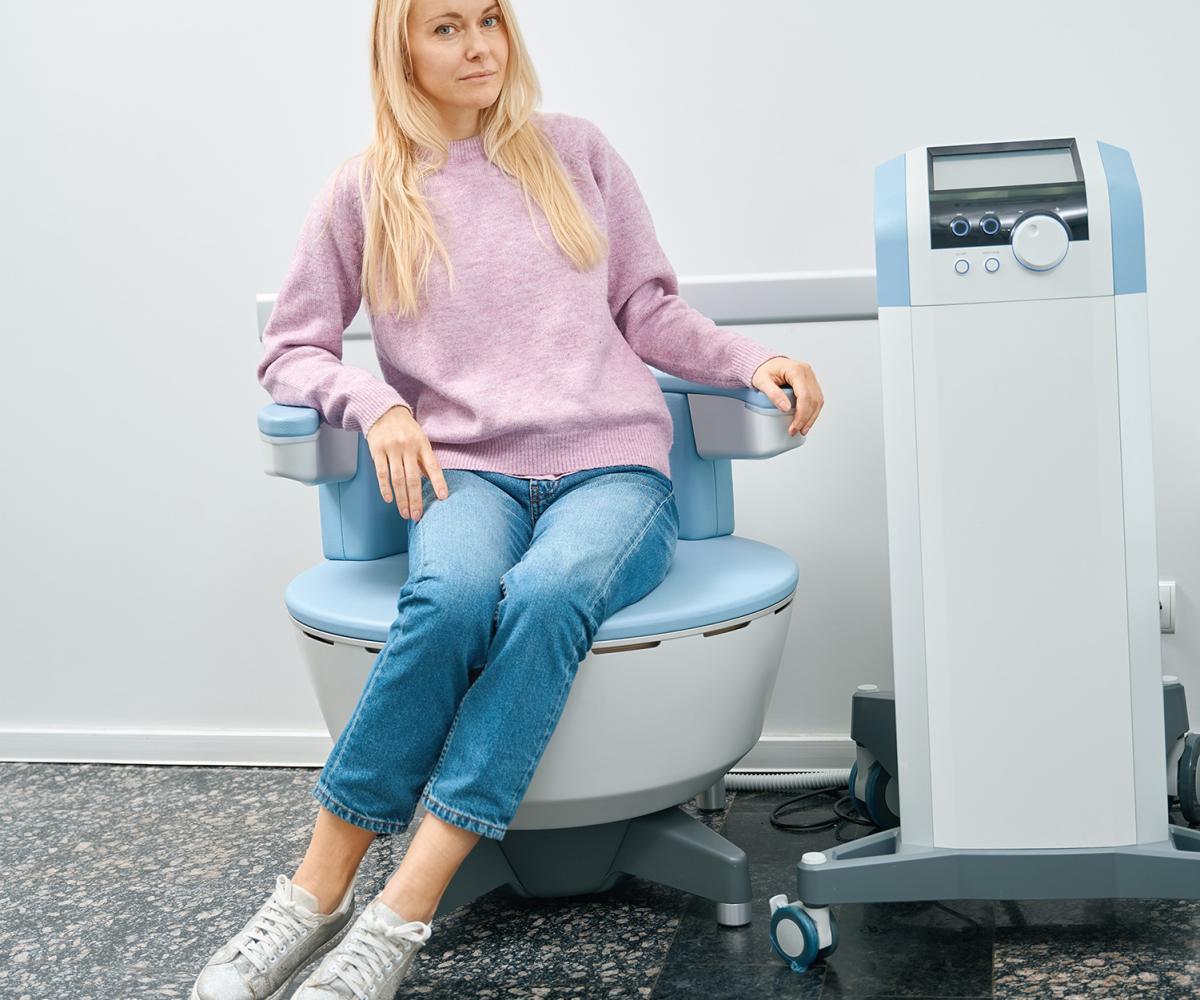
With BTL Emsella you don’t have to think about whether you are doing it right. Under the direction of your specialist clinic, you need only sit comfortably and wait out the treatment. There is no discomfort and rather than have to work on it every day, or twice a day, you will only need twice-weekly appointments.
How can you treat stress incontinence?
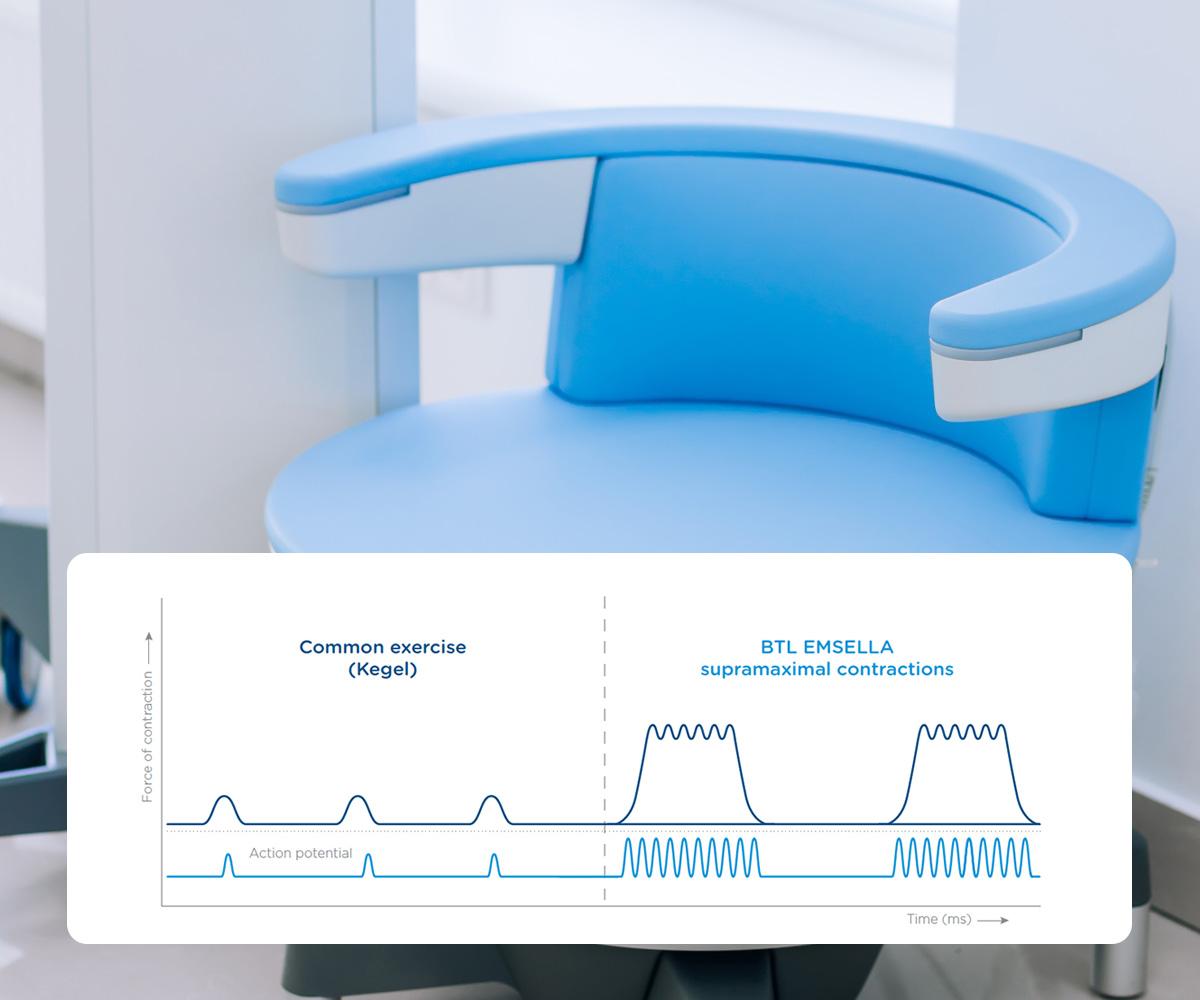
A common treatment for stress incontinence is Kegel exercises which gradually strengthen the pelvic floor muscles by regularly tensing and relaxing them. These can be effective, but are time-consuming and difficult, with slow progress, and for women with particularly weak pelvic floor muscles, are often not possible.
Traditionally, Kegel exercises have been recommended as the most effective non-invasive means of improving pelvic floor muscle strength. Unfortunately, it is difficult for many to identify the correct muscles to work on and maintain the necessary focus. Consequently, the success rate with these exercises can vary anywhere between 30-90%. For those with more severe forms of incontinence, Kegels are not helpful.
Certain risks can occur when Kegels are done incorrectly. From further weakening the pelvic floor muscles to tightening so much as to make intercourse painful, there are many ways this approach can go wrong for a patient.